How will this course prepare you?
The course has been designed and written by opthalmology specialists, read our learning outcomes below.

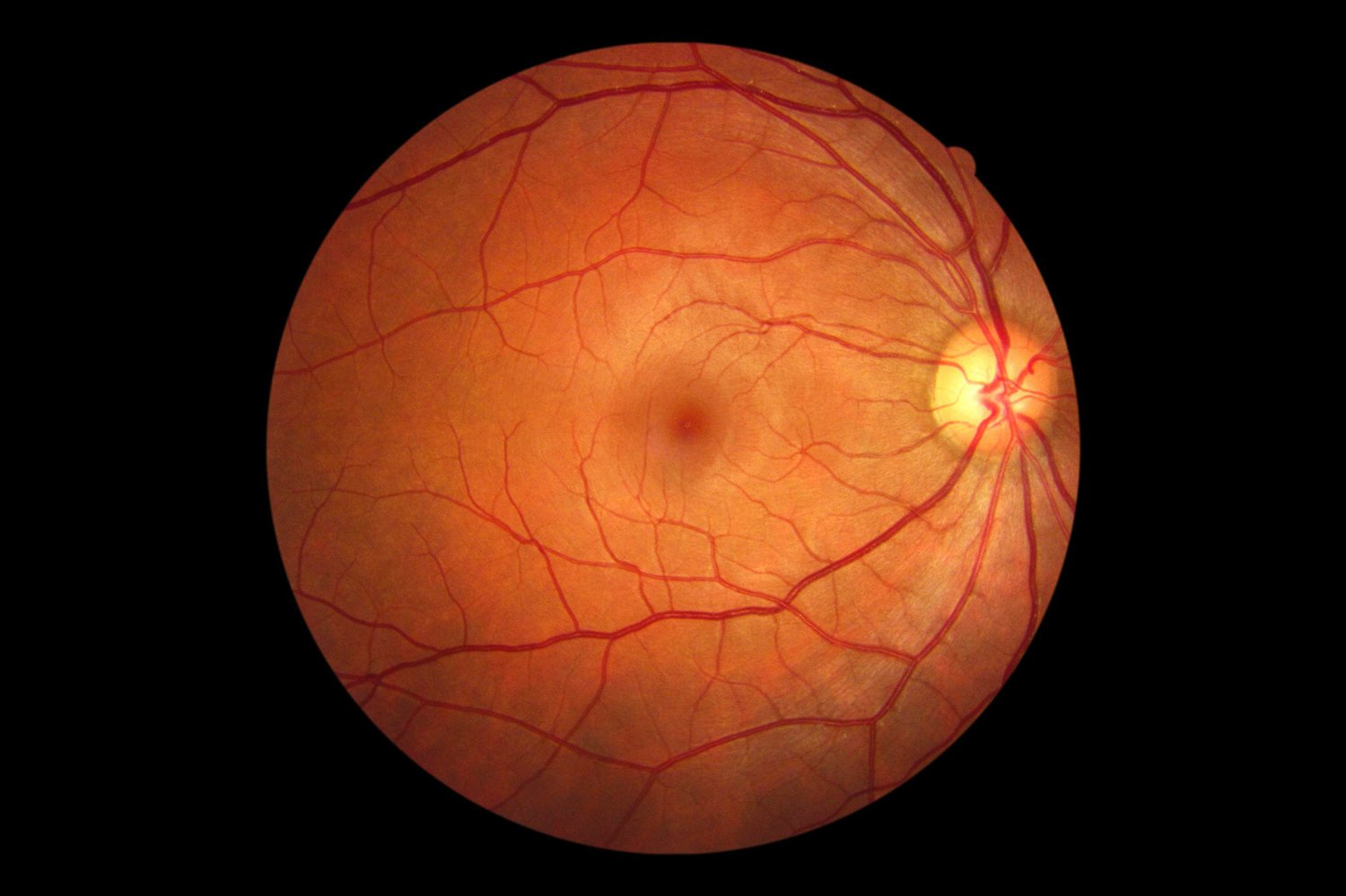
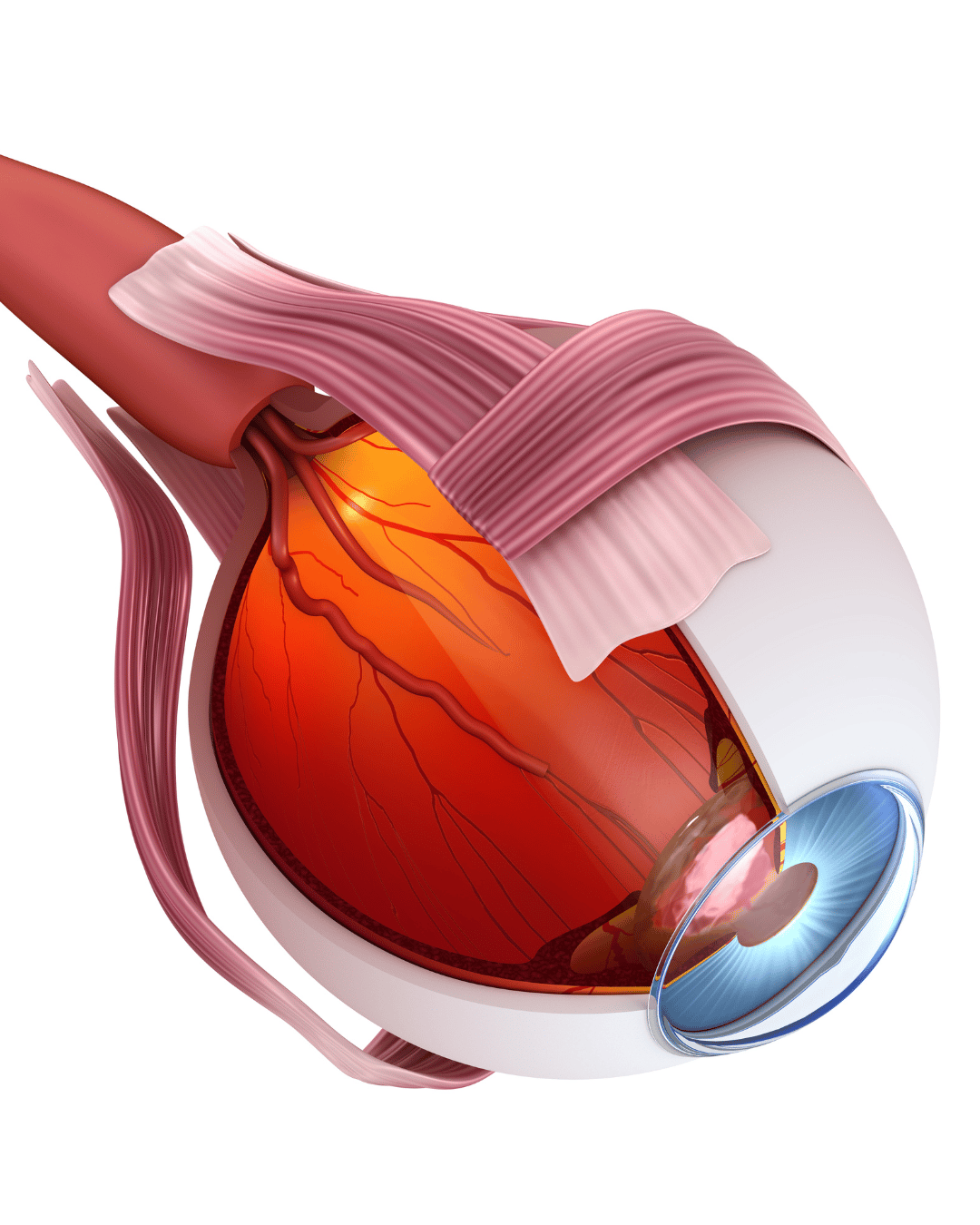
1. Demonstrate a clear understanding of the vascular anatomy of the periorbital and ocular regions, including arterial pathways relevant to dermal filler procedures and the mechanism of filler-induced visual complications.
2. Explain the pathophysiology of vision loss and visual disturbance following dermal filler injection, including how embolisation occurs and which anatomical zones pose the greatest risk.
3. Identify and recognise early signs and symptoms of ocular vascular occlusion, including patient-reported changes in vision and clinical indicators of potential permanent damage.
4. Conduct a structured clinical assessment in the event of suspected visual compromise, including key questions, observational findings, and red flags requiring urgent escalation.
5. Make informed decisions about patient suitability for dermal filler treatment, based on pre-treatment screening, relevant medical history, and individualised risk factors.
6. Communicate vision-related risks effectively during the consent process, including how to explain the risks of blindness and stroke, and how to document meaningful informed consent.
7. Obtain and document consent for the use of hyaluronidase, including its emergency use in periorbital and orbital regions, and explain this clearly and ethically to patients pre-treatment.
8. Perform emergency hyaluronidase injections around high-risk anatomical landmarks, using correct technique, landmarking, and dose selection in a simulated high-pressure scenario.
9. Respond calmly and systematically to a simulated case of vision loss, demonstrating clinical reasoning, effective patient communication, and prioritisation of immediate actions.
10. Describe and reflect on the key medicolegal responsibilities associated with vision-related complications, including how to protect patient safety and support professional accountability.
11. Complete a retrospective clinical note entry using a structured template that includes time-stamped actions, doses, observations, communication, and referral details.
12. Discuss and plan for local escalation or referral pathways by considering available services and developing a proactive plan for emergency access to ophthalmology or acute care.
13. Reflect on personal preparedness and practice protocols, and apply course learnings to improve individual clinical governance, patient safety processes, and complication response planning.